How Psychedelics Work: Neuroplasticity, the Brain & Mental Health Healing
Psychedelic medicines are drawing renewed attention in neuroscience and mental health research because of their potential to help shift deeply ingrained emotional and behavioral patterns. Psychedelic medicines such as psilocybin, LSD, DMT, MDMA, and ketamine are generating great interest in mental health and neuroscience because in many people, they appear to shift long-standing emotional and behavioral patterns, including those with depression, anxiety, trauma, addiction, and end-of-life distress. But how do psychedelics work in the brain?
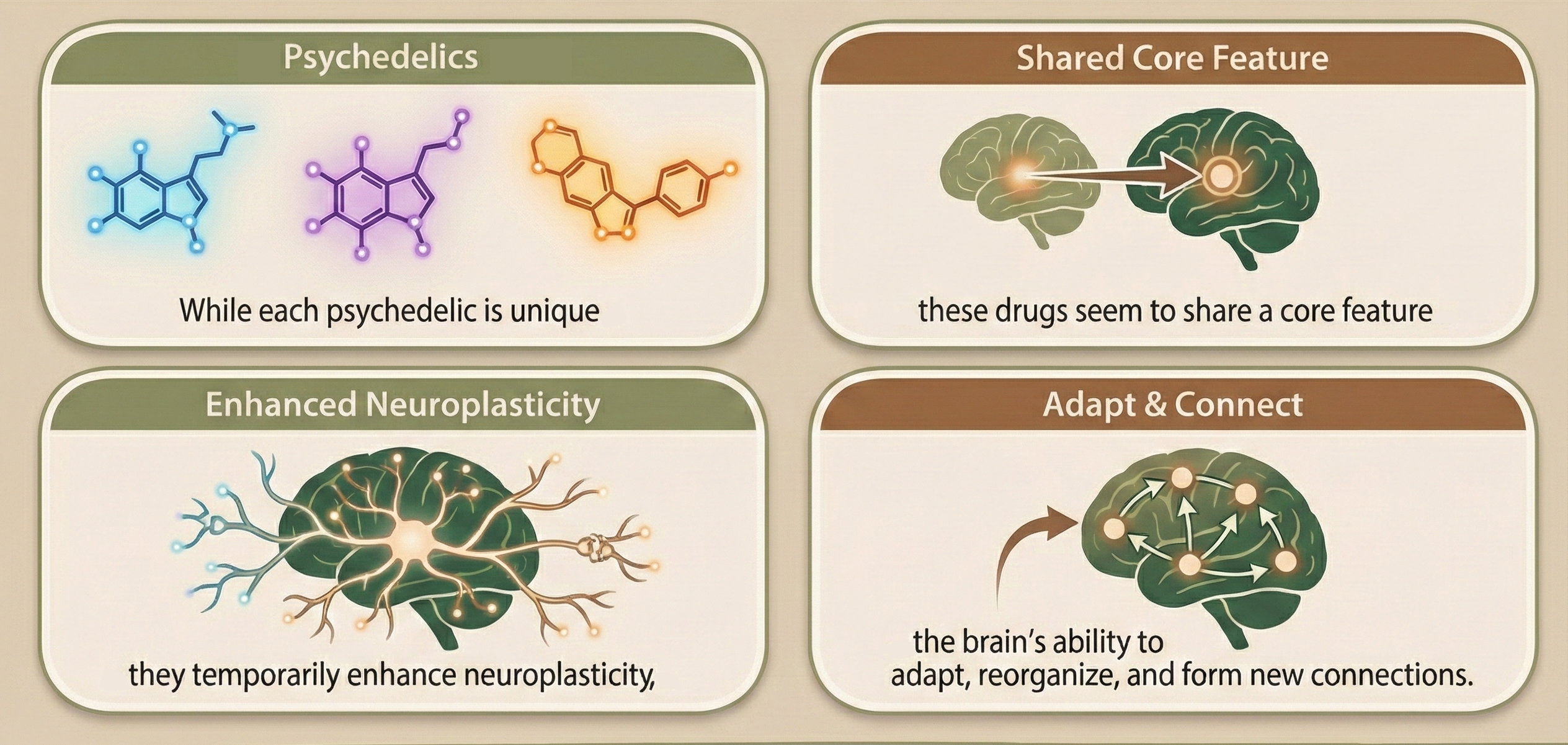
While each psychedelic is unique, these drugs seem to share a core feature: they temporarily enhance neuroplasticity, the brain’s ability to adapt, reorganize, and form new connections. When combined with careful preparation, skilled therapeutic support, and thoughtful integration (collectively known as psychedelic-assisted therapy, or PAT), many studies suggest psychedelics can help open a window for emotional healing, greater cognitive flexibility and durable change.
This article explores the evolving scientific understanding of how psychedelics affect the brain, drawing on decades of clinical trials, neuroimaging research in humans and animals, and advances in our understanding of large-scale brain networks. Together, these findings are helping researchers better understand not only how psychedelics work, but why context, therapy, and support play such a critical role in their potential therapeutic impact.
Classic and Non-Classic Psychedelics
Psychedelic compounds are often grouped into two broad categories based on how they interact with the brain: classic psychedelics and non-classic psychedelics. While these categories reflect different primary mechanisms of action, both appear to influence brain flexibility and emotional processing in ways that may support therapeutic work.
Classic psychedelics, including psilocybin, LSD, mescaline, DMT (the active molecule in ayahuasca) and 5-MeO-DMT (from toad venom and some plants), primarily activate the serotonin 2A (5-HT2A) receptors. This receptor helps regulate perception, cognition, mood, and neuroplasticity, which is why stimulating it can lead to profound shifts in awareness and emotional processing.
Non-classic psychedelics, such as ketamine, MDMA and ibogaine act through different receptor systems but ultimately produce many of the same downstream effects: enhanced neuroplasticity, increased emotional openness, and improved capacity for therapeutic processing.
Ketamine works predominantly through glutamatergic NMDA-receptor modulation, while MDMA increases the release of serotonin, dopamine, and norepinephrine. Ibogaine which comes from the iboga root in Africa, interacts with multiple neurotransmitter systems including serotonin, NMDA, opioid and sigma.
Although these substances differ in their immediate pharmacological targets, research suggests they may converge on shared biological processes related to neural growth and flexibility. For this reason, many psychedelics are increasingly described as neuroplastogens, a term used for compounds that promote synaptic remodeling and, in some contexts, may support longer-term changes in brain connectivity.
What Happens in the Brain:
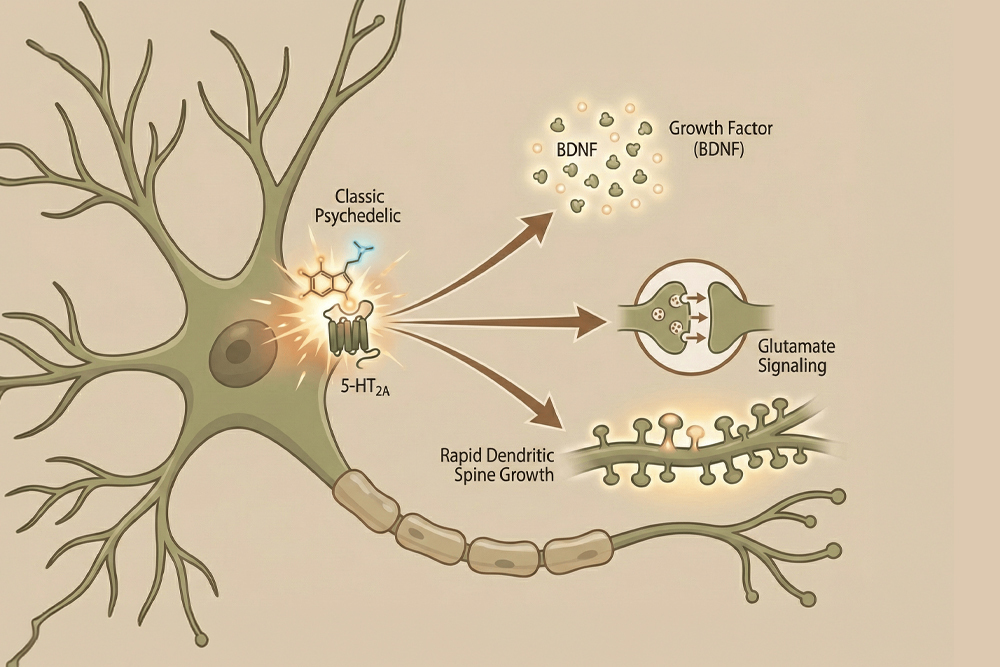
Most classic psychedelics stimulate 5-HT2A receptors on cortical neurons, triggering biological responses associated with flexibility and growth, including:
- increased Brain-Derived Neurotrophic Factor (BDNF)
- altered glutamate signaling
- rapid dendritic spine growth (the tiny connections between neurons)
Together, these changes are thought to temporarily enhance neuroplasticity, allowing brain networks to become more flexible and responsive to new experiences.
In many mental health conditions, including depression, anxiety disorders, trauma-related conditions, and addiction, certain neural circuits can become rigid and self-reinforcing. This rigidity is often associated with repetitive thought patterns, persistent negative beliefs, and limited emotional responsiveness. Psychedelics appear to temporarily loosen these entrenched patterns, creating conditions in which alternative perspectives and emotional responses may become accessible.
Crucially, these biological effects do not operate in isolation. Clinical research suggests that the psychological and therapeutic context in which psychedelics are used plays a major role in shaping outcomes. Guided support during the experience and structured integration afterward may help translate temporary neural flexibility into meaningful psychological change.
It is important to note that while preclinical research is extensive and human neuroimaging studies strongly support similar mechanisms, significant questions remain. Scientists are still working to understand how long psychedelic-induced changes in neuroplasticity last and which factors are most important for sustaining benefits over time.
Rumination & the Default Mode Network (DMN)
One of the most studied effects of psychedelics involves the Default Mode Network. The DMN is a large-scale brain network associated with self-reflection, autobiographical memory, internal narrative, and the construction of one’s sense of identity. It is most active when the mind is focused inward, such as during self-evaluation or repetitive thinking.
In depression and anxiety disorders, recent research suggests the DMN becomes overly rigid, reinforcing rumination and negative self-talk (“I’m broken,” “Nothing will change,” “I can’t trust anyone”).
Psychedelics do not simply “turn off” the DMN, instead they reduce its dominance while increasing communication among brain regions that don’t typically interact. Following a guided psychedelic experience, many individuals report feeling less mentally stuck, more connected to themselves and others, and more emotionally open. This temporary increase in neural flexibility may support meaningful therapeutic work during the experience itself and in the days or weeks that follow, particularly when paired with professional guidance and integration support.
Why Set & Setting Matter
Psychedelic-assisted therapy is a structured therapeutic process, the impact of which depends deeply on context, not just chemistry.
- The term set refers to an individual’s internal state going into a psychedelic session, including mindset, expectations, emotional readiness, and personal intention. Thoughtful preparation helps establish trust and psychological safety, which may reduce distress and support more constructive engagement with the experience.
- Setting refers to the external environment in which the session takes place. This includes the physical space, sensory elements such as music, and the presence of trained clinicians or psychedelic guides who provide support throughout the experience. A calm, carefully designed setting can help contain difficult moments and orient them toward insight rather than overwhelm.
Both set and setting play central roles in shaping how a psychedelic session unfolds. Preparation of one’s mindset builds trust and safety. A calm, well-designed setting helps guide challenging moments toward insight rather than overwhelm. Integration sessions help translate insights into daily life.
The Role of Skilled Practitioners
Psychedelic experiences may bring forward powerful memories, emotions, and deeply personal insights. Trained clinicians provide medical oversight, psychological support, and therapeutic structure to ensure safety and help patients feel grounded, and supported throughout the process.
The work does not end when the psychedelic effects subside. Integration therapy is a critical phase in which clinicians help individuals reflect on their experiences, make sense of insights that emerged, and apply them in daily life. This ongoing therapeutic support plays an important role in transforming temporary experiences into meaningful and sustained psychological change.
How Do Psychedelics Promote Mental Health?
Across many studies, psychedelics appear to help people:
- reduce rumination
- break rigid thought and emotional loops
- open emotional pathways
- increase psychological flexibility
This allows individuals to revisit difficult experiences with less fear and greater compassion. Crucially, the medicine is only part of the equation; enduring transformation arises from the combination of the psychedelic experience and the therapeutic support that surrounds it.
Where PSI and its TRIP Clinics Fit In
At the Psychedelic Science Institute TRIP Clinics in Hollywood and Santa Monica, we are proud to be part of this global movement to better understand brain health and advance responsible psychedelic medicine. Our team is committed to:
- Conducting FDA-regulated clinical trials
- Providing safe, ethical patient care
- Training the next generation of psychedelic practitioners
- Expanding access for underserved communities
We are also committed to being a trusted source of accurate science-based information.
Why This Work Matters
Psychedelic-assisted therapies may represent one of the most promising breakthroughs in mental health and brain health in decades. But progress requires resources, funding for research, training, infrastructure, and access programs. If you believe in this mission, please consider supporting the nonprofit Psychedelic Innovation Fund (PIF). Your donation directly fuels research, education, and patient care.
What This Means for Mental Health Care
Psychedelics are powerful therapeutic tools, not magic bullets. When delivered by experienced clinicians in safe, structured environments, emerging clinical research suggests psychedelic-assisted therapy may enhance neuroplasticity and promote emotional and cognitive flexibility, helping individuals heal from conditions such as major depression, treatment-resistant depression, generalized anxiety disorder, PTSD, addiction, end-of-life distress, and other challenging conditions.
Learn more:
Enrolling Clinical Trials: www.psychedelicsci.com/trials
Ketamine-Assisted Psychotherapy: www.psychedelicsci.com/KAP
PSI Learning Center: www.psychedelicsci.com/learn
Support PIF: www.psychedelicsci.com/pif

.png)
