Default Mode Network and Psychedelics: What Science Shows
.png)
In the growing field of neural network science, one brain system consistently captures fascination, controversy, and sometimes misunderstanding: the Default Mode Network (DMN). In conversations about psychedelics and therapy, the DMN is often portrayed as the seat of rumination, ego, and self-critical loops, something to “break open” during a psychedelic journey. But what is the DMN really? And how do different psychedelics interact with it in ways that might be helpful?
The Default Mode Network is a distributed brain network involved in self-referential thinking, autobiographical memory, and social cognition. Research shows that classic psychedelics such as psilocybin and LSD temporarily reduce rigid connectivity within the DMN, increasing global brain network flexibility. This modulation may support therapeutic outcomes in conditions such as depression, anxiety, PTSD, and addiction when administered in structured clinical settings.
Understanding the Default Mode Network
To understand why the Default Mode Network matters, it helps to look at how this brain system actually operates. It is a distributed network of interconnected areas, including the medial prefrontal cortex, posterior cingulate cortex/precuneus, and lateral parietal cortex, that shows higher activity when the brain is at rest or engaged in self-referential thought. (Neuron)
Key Functions of the Default Mode Network
When we aren’t focused on a specific external task, for example, when we’re daydreaming, reflecting on the past, imagining the future, remembering personal experiences, or thinking about ourselves, the DMN becomes more active. It’s especially involved in:
- Self-referential thinking: forming a coherent narrative about ourselves
- Autobiographical memory: integrating past experiences into identity
- Prospection: imagining future possibilities
- Social cognition: considering others’ perspectives and social meaning
In other words, the DMN helps us understand “where I was” and “where I might be going,” and it plays a crucial role in emotional and social cognition.
The Dark Side of a Good Thing
Default Mode Network overactivity or rigidity can be associated with mental health challenges.
Research shows that excessive or inflexible DMN functioning is linked to:
- Rumination, particularly in depression and obsessive-compulsive disorder
- Over-analysis and worry loops, common in generalized anxiety disorder
- Chronic self-criticism and negative self-referential thinking
- Fixation on past negative experiences
In people with depression and anxiety disorders, for instance, DMN connectivity tends to stay “switched on” in a way that may reinforce negative self-referential loops rather than flexible thinking or adaptive processing.
In this context, the DMN can start to feel like a mental hall of mirrors, not because it’s bad, but because when a system designed for reflection gets stuck, it limits flexibility and exacerbates mental health symptoms.
Psychedelics and the Brain: A Neuroscience Primer
Over the past 25 years, psychedelics have gradually returned to the scientific mainstream as tools for exploring brain function and treating conditions like depression, anxiety, PTSD, and addiction. Central to this research is how these substances affect brain network connectivity, including the DMN. Several landmark neuroimaging studies have shown how classic psychedelics alter brain dynamics:
- Carhart-Harris et al. (2012): One of the first studies to show that psilocybin reduces coordinated activity within the DMN, correlating with subjective experiences of “ego dissolution” and altered self-perception. (PNAS)
- Smigielski et al. (2019): Found lasting changes in self-consciousness and DMN connectivity when psilocybin was paired with mindfulness training, suggesting combined cognitive and neural effects. (ScienceDirect)
- Gattuso et al. (2023): A systematic review concluded that while DMN modulation is a consistent feature across psychedelic studies, its exact role in therapeutic outcomes is still being clarified. (PubMed)
Across studies, a recurring theme emerges: psychedelics don’t “turn off” the DMN, they make it less rigid and less dominantly self-referential, allowing other brain networks to communicate more freely. This shift correlates with increased dynamical repertoire in brain states, potentially underpinning new perspectives and psychological flexibility.
How Different Psychedelics Interact with the DMN
Psychedelics vary in their mechanisms of action, subjective effects, and how they modulate brain networks. Here’s a brief comparison.
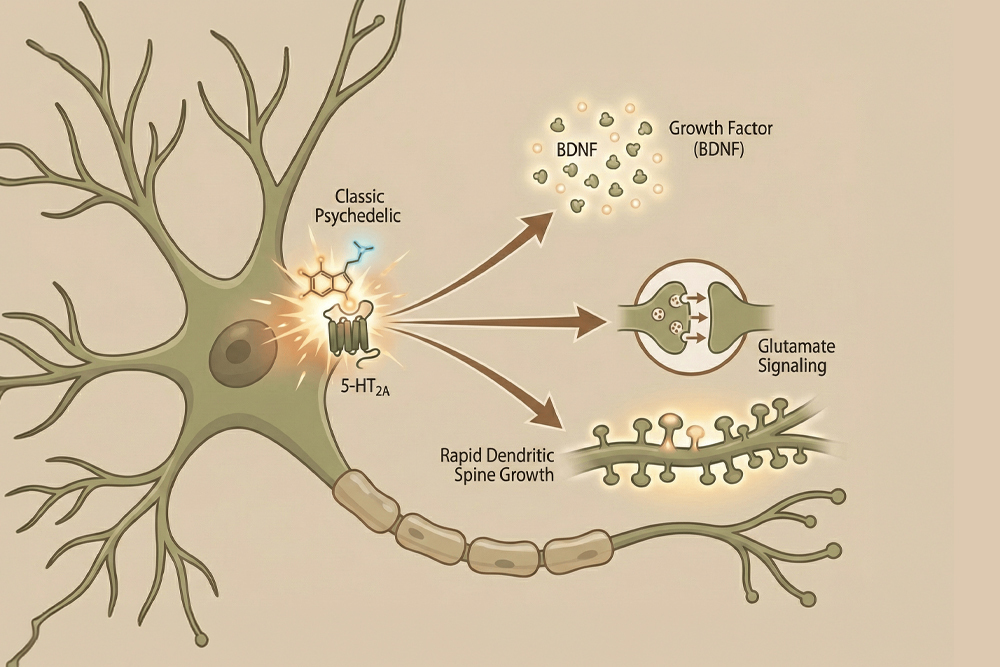
Psilocybin: Psilocybin is a classic serotonergic psychedelic compound found in certain species of mushrooms, sometimes referred to as “magic mushrooms.” It acts primarily on 5-HT2A serotonin receptors. Multiple studies show:
- Reduced within-DMN coherence during acute effects
- Increased global connectivity between other networks, breaking down rigid patterns
- Changes in DMN connectivity persisting beyond the acute experience, potentially linked to enhanced psychological flexibility and mood improvement
- Associated with mystical-type experiences that often correlate with therapeutic outcomes
This modulation may underlie why psilocybin can help people step out of repetitive negative thinking and re-engage with life in a more adaptive way.
LSD (Lysergic Acid Diethylamide): Like psilocybin, LSD is a classic psychedelic with strong 5-HT2A agonism. Notable findings include:
- Decreased directed connectivity within networks, including the DMN, while increasing undirected connectivity across the brain — suggesting a more fluid, less hierarchical brain state. (ScienceDirect)
- LSD tends to produce longer, more intense experiences compared with psilocybin, with rich sensory and cognitive effects.
Both psilocybin and LSD illustrate the principle that reduced dominance of self-referential networks can open pathways to new perspectives.
DMT and Ayahuasca: DMT (dimethyltryptamine) — whether consumed as ayahuasca or vaporized also alters DMN dynamics:
- Functional connectivity patterns reflect a temporary breakdown in typical hierarchical network structure, with effects on self-referential processing. (Cureus)
- Like classic psychedelics, DMT’s impact on the DMN may relate to intense changes in self-perception, time, and meaning — often reported as profound and immediate.
Emerging research (e.g., ongoing fMRI and connectivity studies) continues to clarify how short-acting psychedelics like DMT compare mechanistically with longer-acting ones. (Frontiers)
Ketamine: Pharmacologically distinct from classic psychedelics, ketamine primarily blocks NMDA receptors, leading to rapid antidepressant effects. Its influence on the DMN appears indirect:
- Ketamine disrupts normal functional connectivity patterns, often reducing pathological hyperconnectivity associated with depression
- It also increases global brain connectivity in ways that may underlie rapid mood improvements
Unlike classic psychedelics, ketamine’s subjective effects are typically less mystical but still involve a transient loosening of habitual brain states.
MDMA (Entactogen): MDMA is an entactogen, not a classic psychedelic, with strong effects on serotonin release and emotional processing:
- MDMA doesn’t reduce DMN activity in the same dramatic way as psilocybin or LSD
- Instead, it modulates connectivity between emotion-regulating networks and DMN regions, facilitating increased emotional openness and reduced fear responses
- This is thought to support MDMA’s effectiveness in PTSD therapy, where reconsolidating traumatic memories in a safe emotional context is key
From Network Modulation to Therapeutic Change
Across diverse compounds, a common neuroscientific theme emerges: psychedelics appear to reduce rigid patterns of brain network connectivity, particularly within self-referential systems such as the Default Mode Network.
This doesn’t mean the DMN is “bad.” It’s essential for memory, self-awareness, and planning. But when it becomes too dominant, locked in loops of rumination, worry, or self-criticism, that rigidity may contribute to mental health challenges.
Psychedelics provide a window into how brain networks can be reconfigured, not by erasing the self, but by expanding the space in which the self can be re-examined, reorganized, and integrated.
DMN Is Not the Enemy, It Is the Context
The Default Mode Network is a central neural hub for introspection, memory, social cognition, and self-identity. Its activity is neither inherently good nor bad, but its rigidity can be associated with mental health challenges. Psychedelics, from psilocybin to ketamine, transiently dampen or reconfigure DMN dynamics in ways that may facilitate therapeutic breakthroughs when combined with expert support and intention.
Rather than seeing the DMN as the “seat of ego gone wrong,” it’s more accurate to view it as a flexible system that sometimes needs loosening, not elimination.
The science is evolving, and with it, our understanding of how psychedelics can support healing somewhere between neurons and meaning.
Where PSI and its TRIP Clinics Fit In
At the Psychedelic Science Institute TRIP Clinics in Hollywood and Santa Monica, we are proud to be part of this global movement to better understand brain health and advance responsible psychedelic medicine. Our experienced team is committed to:
- Conducting FDA-regulated clinical trials
- Providing safe, ethical patient care
- Training the next generation of psychedelic practitioners
- Expanding access for underserved communities
We are also committed to being a trusted source of accurate science-based information, helping the public separate hype from reality.
Why This Work Matters
Psychedelic-assisted therapies may represent one of the most promising breakthroughs in mental and brain health in decades. But progress requires resources, funding for research, training, infrastructure, and access programs.
If you believe in the potential of this science to change lives, please consider supporting the nonprofit Psychedelic Innovation Fund (PIF). Your donation directly fuels research, education, and patient care. Together, we can help usher in one of the most transformative eras in mental healthcare in over half a century.
FAQs
What does the default mode network do?
The default mode network supports self-reflection, autobiographical memory, and imagining the future. It becomes active when the brain is not focused on an external task.
Why is the default mode network linked to depression?
In depression, the DMN can become overly rigid and hyperconnected, reinforcing patterns of rumination and negative self-referential thinking.
Do psychedelics turn off the default mode network?
No. Research suggests psychedelics reduce rigid connectivity within the DMN rather than turning it off entirely. This allows other brain networks to communicate more freely.
Which psychedelics affect the DMN?
Psilocybin, LSD, and DMT directly alter DMN connectivity through serotonin receptor activity. Ketamine and MDMA influence related networks through different pharmacological mechanisms.
Are changes in the DMN permanent?
Most changes are transient during the acute experience. Some studies suggest longer-term shifts in connectivity may occur when psychedelic therapy is combined with structured psychological support.
Learn more:
Enrolling Clinical Trials: www.psychedelicsci.com/trials
Ketamine-Assisted Psychotherapy: www.psychedelicsci.com/KAP
PSI Learning Center: www.psychedelicsci.com/learn
Support PIF: www.psychedelicsci.com/pif